
Glaucoma is one of the leading causes of preventable blindness in Aotearoa. Yet most people who have it don’t even know it’s there—until permanent vision loss has already begun. The good news? With early detection and the right care, most glaucoma‑related blindness can be prevented.
What Is Glaucoma?
Glaucoma damages the optic nerve—the vital “cable” that connects your eye to your brain. This usually happens when pressure inside the eye becomes too high. The damage starts quietly in your side vision, creeping in until it affects central sight. Once vision is lost, it can’t be restored—making early detection absolutely crucial.
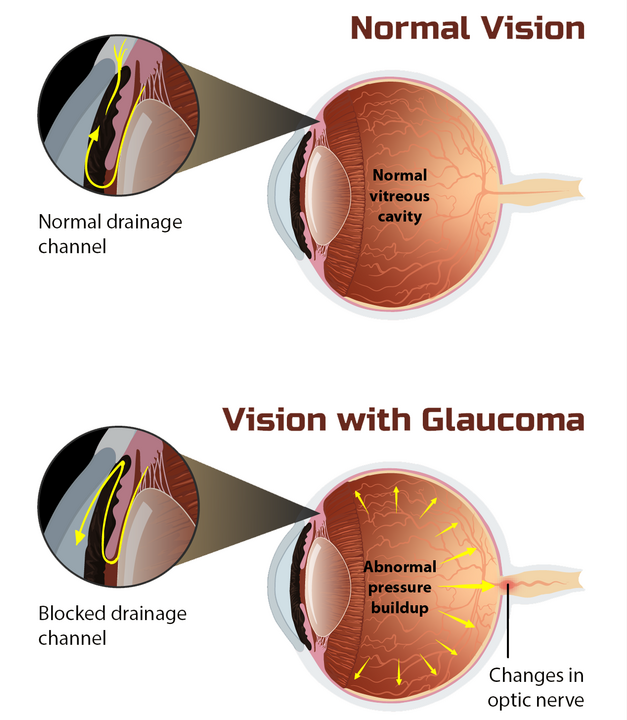
Types of Glaucoma
- Primary open‑angle glaucoma:
The most common form. Slow, subtle, and often symptom‑free until major damage is done. - Angle‑closure glaucoma:
A sudden, painful emergency with blurry vision, halos, headache, or nausea. Urgent specialist care is vital. - Normal‑tension glaucoma:
Optic nerve damage even when eye pressure appears normal—often linked to blood flow issues. - Secondary glaucoma:
Caused by inflammation, long‑term steroid use, pigment or debris in the eye, or diabetes‑related blood vessel changes.
Who Should Pay Extra Attention?
You’re at higher risk if you:
- Are over 40 (risk jumps again after 70).
- Have a parent or sibling with glaucoma.
- Have high eye pressure, thin corneas, myopia, or hyperopia.
- Have poor blood flow regulation.
- Are Māori or Pasifika—groups more likely to be under‑diagnosed.
If you’re in any of these groups, an eye exam isn’t optional. It’s essential.
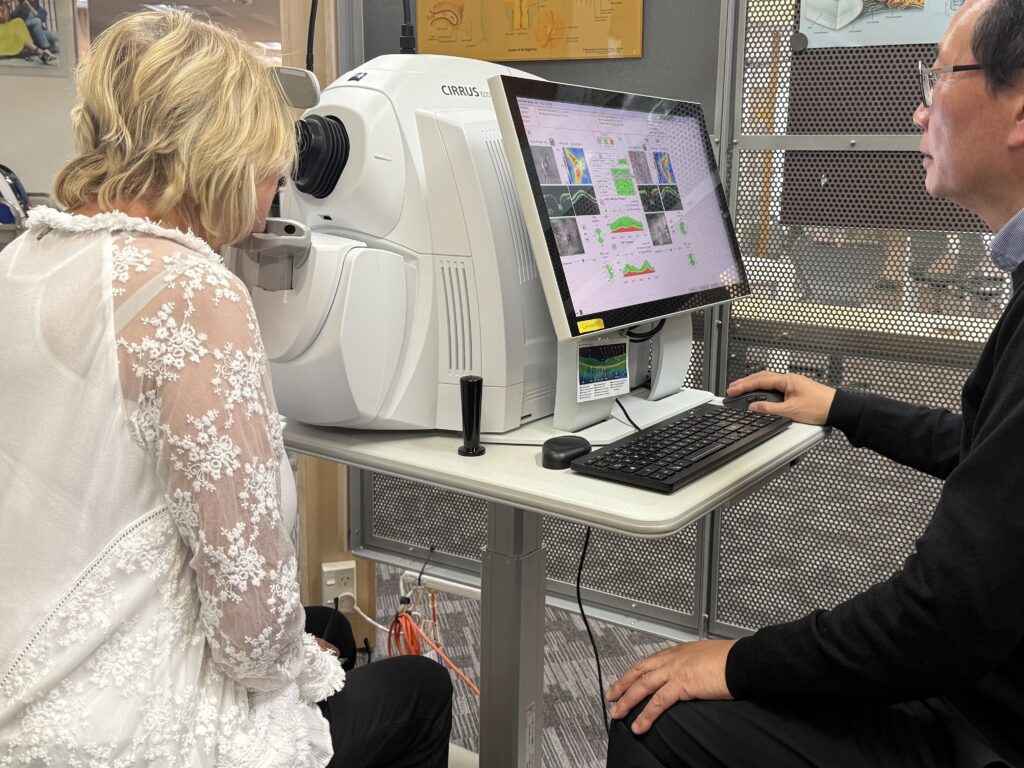
How Optometrists Spot It Early
Even without symptoms, optometrists can pick up the earliest signs by examining:
- The appearance of the optic nerve (cup‑to‑disc ratio, notching, small haemorrhages).
- Thickness of the retinal nerve fibre layer using OCT scanning.
- Your peripheral vision using visual field testing.
Regular monitoring allows subtle changes to be caught before they affect how you see day to day.
Symptoms—Often Too Subtle to Notice
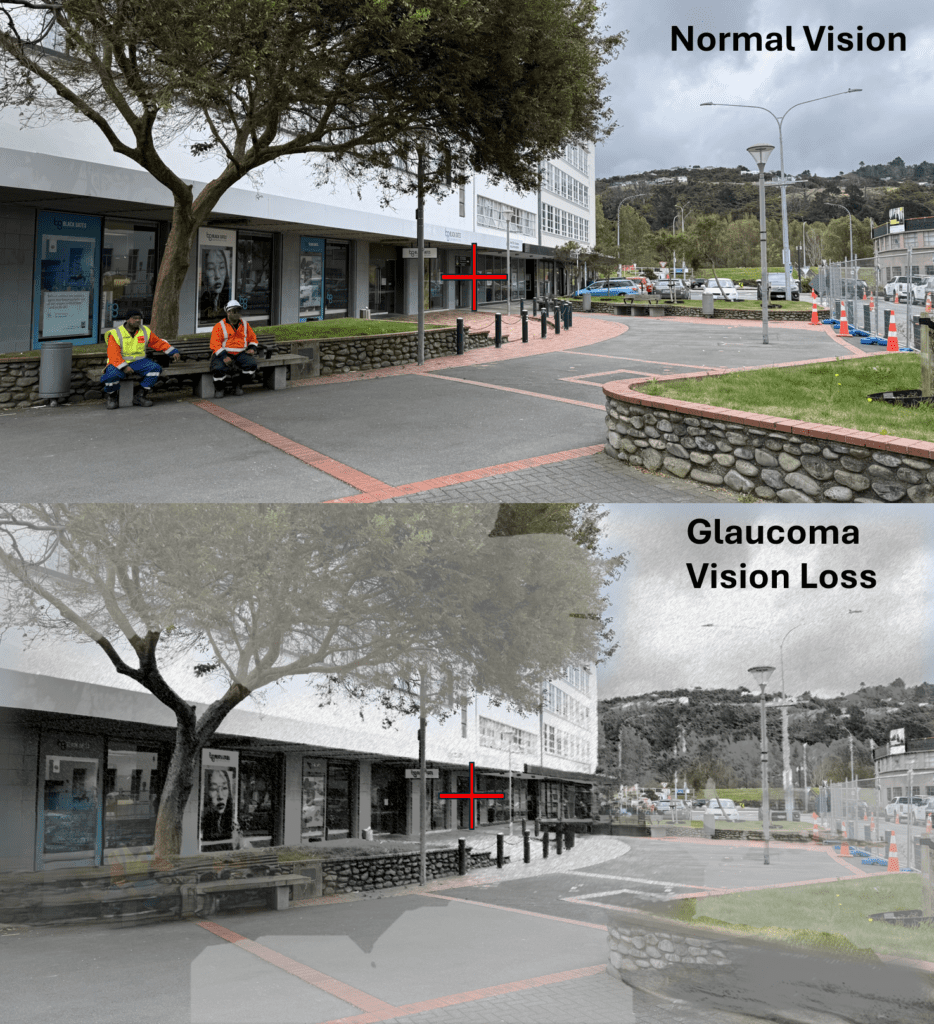
Most people feel completely normal until glaucoma is advanced. Later you might notice:
- Difficulty driving at night.
- Bumping into objects on the side.
- Blurry central vision in late stages.
Don’t wait for symptoms—glaucoma usually doesn’t give you any.
Treatment That Protects Your Sight
While there’s no cure, treatment can slow or stop further damage:
- Prostaglandin analogue eye drops (like latanoprost) used once nightly can lower pressure by 20–30%.
- Selective Laser Trabeculoplasty (SLT): A quick, effective laser treatment that improves drainage and may reduce or eliminate the need for drops.
- Other medications like beta blockers, alpha agonists, or carbonic anhydrase inhibitors may be added.
Regular follow‑ups are key, these typically include pressure checks, OCT scans, and visual field testing to ensure the treatment is working.
Driving and Glaucoma in NZ
Glaucoma can reduce peripheral vision—critical for safe driving. If field loss is detected, you may need an Esterman binocular field test to meet Waka Kotahi NZTA standards. Talking early with your eye specialist helps you stay safe and prepared.
Where to Get Support
- Glaucoma New Zealand (glaucoma.org.nz): Free resources, education, support, and advice.
- RANZCO: Provides clinical guidelines for eye care in NZ.
- Healthify.nz: Clear explanations and practical help.
- Your optometrist: Often the first line of defence and your partner in protecting your sight.
The Bottom Line
Glaucoma often has no early symptoms, but early detection can save your sight. If you’re over 40—or have any risk factors—book an eye exam. It could be one of the most important health checks you ever do.

